Institutionalized Racial Bias in Public Health: Inferior Care, Callous Disregard & Increased Deaths
“Whether it’s unconscious, explicit, institutional or research bias, discrimination in the health care system contributes to the stark disparities seen in how COVID-19 sickens and kills patients of color, health care experts agree.” USA Today
The following draws on numerous investigative reports by ProPublica – including today’s scathing expose of the culpability of New York State Governor Andrew Cuomo, whose March 25th directive sentenced thousands of elderly residents at nursing homes to death. Other reports drawn on include: USA Today, Kaiser Health News, SCIENCE, Health Affairs, The New York Times, The Washington Post as well The CUT…
In October 2019, the journal SCIENCE published a study by a team of Harvard and the University of California, Berkeley, who reported evidence of systemic racial bias in an algorithm that is widely used by hospitals to identify the health needs of patients. Use of this algorithm has resulted in under calculating the medical care needs of Black patients. The biased miscalculation is due to the choice of medical expenditure as the data that was calculated in the algorithm. Because Black people cannot afford expensive treatments, they generate fewer healthcare expenditures; therefore, their medical needs have been grossly miscalculated.

A 2017 ProPublica investigation analyzed two years of hospital discharge data from New York, Illinois and Florida. The investigators found growing evidence that the poor quality of care at hospitals where a disproportionate number of Black women deliver babies, is an important contributing factor in the disparity between the high death rate of Black women in childbirth-related causes – which is more than three times as high compared to white women. In New York City, where the overall maternal mortality rate across the city has dropped, the disparity between White and Black women who die has increased.
Dacheca Fleurimond, died of hemorrhage complications after giving birth to twins at SUNY Downstate hospital in Brooklyn. ProPublica reported that:
“On average, 34 percent of women who hemorrhage while giving birth at New York hospitals experience significant complications. At SUNY Downstate, it’s 62 percent.
Medical Bias, Racial Discrimination in Healthcare is a USA Today report (June 15, 2020) that describes a litany of medical treatment disparities based on race. The healthcare hierarchy in hospitals is inhospitable and insensitive to Black patients.
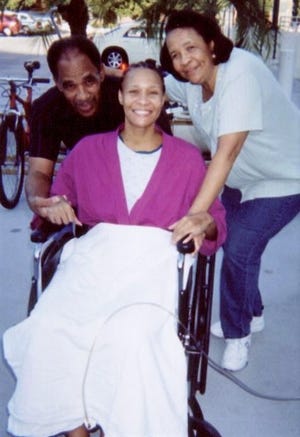
Actress Alicia Cole (shown with her parents) developed flesh-eating disease, sepsis and three life-threatening antibiotic-resistant infections after what was supposed to be a minor surgery in 2006. But for all she went through, Cole recalls details of the racial bias she encountered at the hospital as clearly as the physical ones she suffered.
An example of disparity of care is how Black women with uterine fibroids are treated differently than white women. While an estimated 70% of women will have uterine fibroids – benign tissue masses in or around the uterus – in their lifetimes, most are benign and nothing need be done. If they cause pain and discomfort, they can be easily removed with minimally invasive laparoscopic surgery.
Black women, however, are at far greater risk than white women of being encouraged – even those of childbearing age – to have a major surgical procedure to remove the uterus as well as the fibroids in a hysterectomy. This sterilizing surgical procedure has been the standard of gynecological care for fibroids in the US for many decades.

USA Today reporters Jayne O’Donnell and Ken Alltucker note that the “choice” given to Black women “sounds like echoes of the forced sterilization of many Black women up until 1972, it feels that way to women faced only with the hysterectomy option.”
Dr. Soyini Hawkins is one of very few Black medical doctors, she provides Black women in the Atlanta area fibroid treatment options.
CNBC reported on May 14, 2020: “In Louisiana, where black people make up about 33% of the population, Gov. John Bel Edwards said in early April they account for more than 70% of the state’s coronavirus deaths, with the majority of these fatalities taking place in New Orleans. And in New York City, black and Latino people are twice as likely to die from the virus than their white peers. according to data by the local government. All of these figures are based on the most recent data released to the public, with more states and local governments being pressured to share a racial breakdown of their numbers.”
Kaiser Health News reported evidence of Long-Standing Racial And Income Disparities Seen Creeping Into COVID-19 Care (April 2020), A biotech firm review of billing information found that black people who visited hospitals with Covid-19 symptoms in February and March were less likely to get tested or treated than white patients.
“Delays in diagnosis and treatment can be harmful, especially for racial or ethnic minority groups that have higher rates of certain diseases, such as diabetes, high blood pressure and kidney disease. Those chronic illnesses can lead to more severe cases of COVID-19.

The New York Times reported on May 20, 2020, how bias affected Black families during the Covid-19 pandemic
“Decades of research shows that black patients receive inferior medical care to white patients. A long history of experimentation, exploitation and mistreatment has left many African-Americans deeply suspicious of the medical establishment. Now comes Covid-19, and the fear among many families […] that racial bias might be contributing to the disproportionately high rate at which the novel coronavirus is killing African- Americans[…]
The Washington Post reported that a civil rights group and hundreds of doctors called on the federal government to release race and ethnicity data on coronavirus infections and deaths from covid-19, citing reports that the pandemic is affecting African Americans at a disproportionate rate. The Centers for Disease Control (CDC) and most state health departments have withheld information about the race and ethnicity of those who have tested positive for or died of covid-19. A Yale University study found that mortality for Blacks is 3.57 times higher than for whites.
In a letter to Secretary Alex Azar, Secretary of Health and Human Services, Lawyers’ Committee for Civil Rights Under Law, demanded the release of ethnic Covid-19 data. They cited civil rights laws that prohibit health-care providers “from using federal funds to administer healthcare services that discriminate on the basis of race, color, or national origin.”
In New York City, deaths per 100,000 from the coronavirus (adjusted for the size and age of the population) have disproportionately affected Hispanic and black people.
Hispanic……………………………………………22.8
Black……………………………………………19.8
White……………………..10.2
Asian……………….8.4
Public officials claimed that lockdown was needed “to protect the vulnerable elderly.” However, those policy directives devastated the economy and actually increased the number of deaths among the elderly people in nursing homes and senior care homes. US, government directives caused the death of tens of thousands of human lives – these include the lives of elderly residents and the lives of their care givers, who lacked protective gear, and were mostly people of color.
As ProPublica reports: “Fire Through Dry Grass”: Andrew Cuomo Saw COVID-19’s Threat to Nursing Homes. Then He Risked Adding to It

On March 25th New York State Governor Andrew Cuomo and his health commissioner, Howard Zucker, MD, issued a directive that ordered nursing homes to admit residents whether or not they were infected with coronavirus – even when these facilities lacked personal protective gear for staff, and lacked resources to separate and protect uninfected residents from those infected.
ProPublica reports that NYS is the only state in the nation that forbade testing those who were being placed or returned to nursing homes. As a result of Cuomo’s directive, “COVID=19 tore through New York States’ nursing facilities, killing more than 6,000 people. In all, as many as 4,500 COVID-19 infected patients were sent to nursing homes across the state.”

The Society for Post-Acute and Long-Term Care Medicine, known as AMDA, had warned from the beginning that Cuomo’s order admitting infected patients posed a “clear and present danger” to nursing home residents. Now, Jeffrey N. Nichols, who serves on the executive committee of the group, said “the effect of that order was to contribute to 5,000 deaths.”
Andrew Cuomo and Howard Zucker are responsible – and should be held accountable. In Cuomo’s own words, he caused the spread of “Fire Through Dry Grass” — only those were living human beings, not “dry grass”.
A further demonstration of state officials’ callous disregard for the lives of the elderly, ProPublica reports that after the March 25th directive, they failed to monitor the consequences of their directive:
“The state Health Department did not track in real time what happened when COVID-19 patients were transferred from hospitals to nursing homes. One senior nursing home industry official said the state Health Department didn’t even begin comprehensively counting COVID-19 deaths in these facilities until well into April, although the department has disputed that claim.”
Charles Branas, who leads the epidemiology department at Columbia University’s Mailman School of Public Health stated: “the policy could well have increased New York’s COVID-19 death toll by a magnitude that will be determined by future researchers. If you introduce 4,500 people sick with a potentially lethal disease into a vulnerable and notoriously imperfectly monitored population, people are apt to die.”
Steven McLaughlin, the Rensselaer County Executive, said of the deaths at Diamond Hill nursing home were “Uncalled for, unnecessary, should never have occurred, and wouldn’t have but for a tragically misguided order from the state.” He called Cuomo “a bully who ran from responsibility when his policies went awry.”
- ProPublica reports that “Documents show Zucker, the health commissioner, was fully aware of events at Diamond Hill and reassured local leaders that the department had offered help moving patients to other facilities, but was told it wasn’t needed.”

Stephanie Gilmore, a former nurse at the Diamond Hill nursing home outside Albany. She is the whistleblower who was confronted with the March 25th NYS directive which she was instructed to keep secret. She and another former nurse told ProPublica the facility was chronically short of staff and equipment. Sometimes the facility had as few as four aides and one nurse looking after as many as 80 patients on a single floor, each suffering a variety of ailments that screamed for attention — incontinence, dementia, basic mobility. She sent an email in all capital letters to the owners, with the subject line: ATTEMPTING TO DO THE IMPOSSIBLE!
“As a nursing professional, it’s unsafe to admit residents into the facility when we are critical with staffing and unable to care for the residents already in the building… I have tried to assist in any way that I can, however I am being stretched way too thin.”
When the situation did not improve, but deteriorated even more, she called the county Health Department and she complained to Ari Grinspan, the CEO of Diamond Hill. She was fired for raising her human and professional concerns about the dangerous conditions at the nursing home.
- The coronavirus pandemic is also being used by hospitals to put into practice discriminatory racial profiling policies.
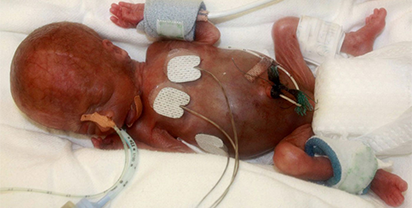
In a move that has received little attention, hospitals around the country have been separating newborns from mothers who are “suspected” of being infected with COVID-19. Whereas the World Health Organization, the Society of Gynecology and (SOGC), the Canadian Paediatric Society, the Royal Australian and New Zealand College of Obstetricians and Gynaecologists emphasize the documented benefits of keeping newborn infants with their mother,
CDC guidelines recommend: “temporary separation of the newborn from a mother with confirmed or suspected COVID-19 should be strongly considered to reduce the risk of transmission to the neonate.” The American Academy of Pediatrics added its “authority” recommending strict separation. CDC, however, acknowledges that: “decisions about temporary separation should be made in accordance with the mother’s wishes.”
The American College of Obstetricians and Gynecologists takes a more humane and evidence-based position:
“Given the limited evidence on this topic, the determination of whether to keep patients with known or suspected COVID-19 and their infants together or to separate after birth should be made on a case-by-case basis, using shared decision-making between the patient and the clinical team. In the counseling process, it is important to include a discussion of the risks and benefits, including the benefits of keeping the mother with the newborn and the risk of uncommon but potentially severe infection. Although separation in the hospital setting temporarily reduces the risk of neonatal infection, separation of patients from their newborns may be linked to additional risks including, but not limited to, undue stress on the patient and disruption of breastfeeding.”
Many hospitals across the US are dictating that newborns be separated “until the mother is known to be negative” – sometimes for up to a week or more – without regard for the harm this may cause infant and mother. Indra Lausero, a staff attorney at the National Advocates for Pregnant Women, said: “In my work, I already see how hospitals make policies that don’t always take into account families’ needs, people’s psychological well-being, or even the specific needs of newborns with regards to bonding and attachment.” Some hospitals separate a newborn from a mother who tests positive for substance use.
Another ProPublica, report reveals that a major hospital in Albuquerque, NM – Lovelace –separated Native American newborn infants from their mothers according to the mother’s residence Zip Code.
LaToya Jordan, describes her ordeal at Long Island’s NYU hospital

“They Separated Me From My Baby. I never saw her further than my knee. Not touching or seeing my child’s face, no skin-to-skin — I cried a lot about that.” She said she wasn’t allowed to take a video of her daughter being bathed at a distance, or even glimpse her in the nursery through a window. I get that everyone is overwhelmed, but I didn’t feel like a patient. I felt like I was a damn near criminal.” Jordan, who has her own organizational and leadership consulting practice, said “It felt so inhumane.”
12 hours after she gave birth, LaToya Jordan was told she tested positive for COVID-19, and the next day she was discharged without her baby. The next day, her daughter tested negative and LaToya was allowed to hold her baby daughter for the first time and she was allowed to take her home.
- If the infected mother was allowed to take her uninfected infant home, why, then, was she separated from her infant after birth in the hospital? Did the staff have any idea about the purpose of the separation order that they implemented?
A report in ProPublica, reveals that Lovelace, a major hospital in Albuquerque, NM separated Native American newborn infants from their mothers — according to the zip code of their residence.
A Systematic Review Of The Food And Drug Administration’s ‘Exception From Informed Consent’ Pathway published in Health Affairs, in 2018. The authors, by William Feldman, Spencer Phillips Hey, and Aaron Kesselheim, reviewed the complete FDA docket of 41 trials exempted from informed consent requirements. Among the 46,964 patients in the review, 96% were enrolled without consent. “Nearly one-third of US patients in EFIC trials were African American.” Two (8%) of the 24 superiority trials demonstrated a benefit from the experimental interventions. The reviewers report that “many interventions were associated with adverse effects, including increased mortality, neurological deficits, and myocardial infarctions.”
The fact that fewer than 1% of these non-consenting human subjects withdrew before the primary endpoint, raises the specter that the human beings in the trials were prevented from withdrawing. They were, in a real sense, captives of experiments.
 Adverse Events: Race, Inequality, and the Testing of New Pharmaceuticals by Jill Fisher (April 2020) is the culmination of a 5-year research project that involved interviewing 268 volunteers and staff across the U.S. Fisher explores the social inequalities that shape Phase I trials in fundamental ways: those who volunteer “are typically recruited from African American and Latino/a communities,” an underclass whose desperate economic circumstances induce them to volunteer, usually as “serial volunteers.” She observes that medical research is an enterprise in which nearly everybody involved is incentivized to game the system.
Adverse Events: Race, Inequality, and the Testing of New Pharmaceuticals by Jill Fisher (April 2020) is the culmination of a 5-year research project that involved interviewing 268 volunteers and staff across the U.S. Fisher explores the social inequalities that shape Phase I trials in fundamental ways: those who volunteer “are typically recruited from African American and Latino/a communities,” an underclass whose desperate economic circumstances induce them to volunteer, usually as “serial volunteers.” She observes that medical research is an enterprise in which nearly everybody involved is incentivized to game the system.
Fisher identifies a major flaw in Pharma’s clinical trial enterprise; the fly in the ointment is that these underprivileged “healthy volunteers” who desperately need the money, skirt the rules about the length of time they wait between trials: “by moving from clinic to clinic-these serial participants can end up affecting the validity of the trials themselves”
This is because the drugs they ingested in the previous trial are likely to affect their response to the next drug that is being tested. Fisher shows how the exploitation of racial and societal inequalities are intertwined with pharmaceutical testing which is a signal that the dangers posed by this research enterprise exploits the economic and social inequality of those who volunteer and uses invalid data that may undermine public health.
Institutional Racism by Shirley Better was first published in 2002. In the enhanced 2007 second edition, she explores the  historical origins of institutional racism, details its devastating effects on contemporary society such as the aftermath of Hurricane Katrina, and outlines real possibilities for social, political, and economic change in the 21st century.
historical origins of institutional racism, details its devastating effects on contemporary society such as the aftermath of Hurricane Katrina, and outlines real possibilities for social, political, and economic change in the 21st century.
Dr. Better received her MSW from University of Michigan and her doctorate in Social Welfare from UCLA. She recently retired as a full time professor in the School of Social Work at California State University at Los Angeles. During her tenure at the University, she served in administrative roles as well as classroom teaching. She served as Dean of the Office of Continuing Education, Director of the Associated Clinics, and was Chair of the Department of Social Work for many years. She founded and Chaired the University Caucus of African American Faculty.